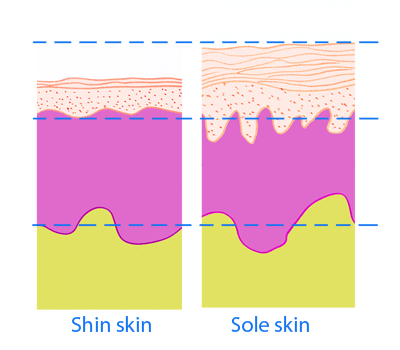
No matter how well a prosthetic limb is fitting, it still applies load through skin and soft tissues that are not meant to be mechanically loaded. An example of this is to compare the skin on sole of your foot to that of your shin. You can see that the skin is thicker and firmer on the load bearing surface of the foot.
The simplified diagram above shows a two slices of skin under a microscope. The skin of the sole looks more ‘reliable’.
When wearing an artificial limb, the skin is at a higher risk of conditions which should be treated by medical professionals. Below is a list of the most common skin issues experienced by limb wearers. If you believe you may have one of the following disorders, we strongly recommend that you consult your Prosthetist and GP about your individual situation.
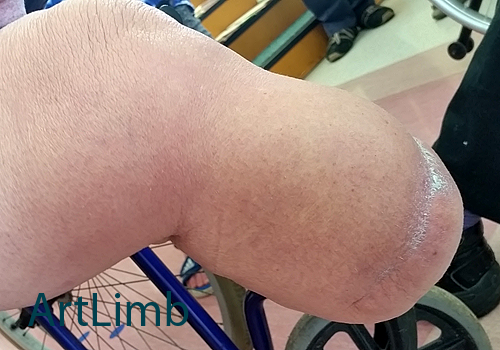
Oedema is an accumulation of excessive fluid in the soft tissues. Redness or mild oedema frequently occurs when a prosthetic limb is first worn. This condition can often be managed by using shrinker socks or elastic bandages when the prosthesis is off. A proper fitting prosthesis needs to be worn to prevent oedema occurring and limit its progression. If unattended, the condition can lead to complications.
The photo above shows a stump effected by oedema.
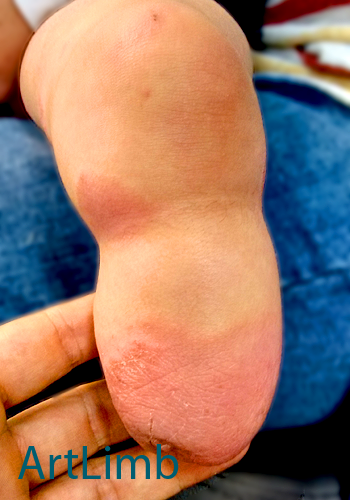
Contact dermatitis is an inflammatory skin reaction to contact with irritants or allergens. It usually presents as redness, blisters, swelling and itching. Before contacting your GP, it is important to find out from your prosthetist what materials are in contact with your skin. This will help your GP to target their treatment which usually involves medications and avoiding the substance causing the dermatitis (this can be certain prosthetic material, cleaning products, contamination, etc).
The photo above shows a stump effected by dermatitis.
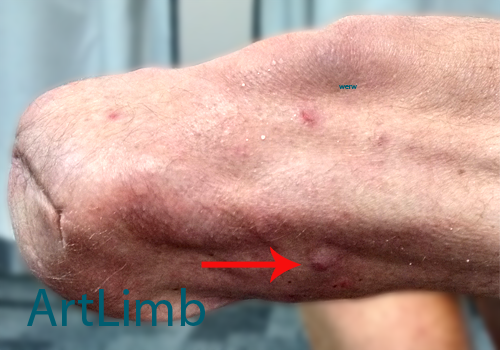
Epidermoid cysts/Inflamed sweat glands are often a chronic condition most likely to be seen in areas where the prosthetic socket applies local pressure to the soft tissue causing inflammation. The prosthetic socket may need to be adjusted and the stump may need medical treatment. Treatments may include antibiotic therapy, improved hygiene regime or in some cases excision of the cyst (surgical removal).
The photo above demonstrates the area of the stump with a cyst under thinned skin which looks like a small lump.
Bacterial folliculitis is inflamation of the hair folicles (openings of the skin that enclose hair). This can be caused by poor hygiene of the stump in combination with excess sweating and mechanical load in the prosthetic socket.
Treatment may involve improving the hygiene regime and medical treatment for infection.
The photo above demonstrates the area of the stump with folliculitis.
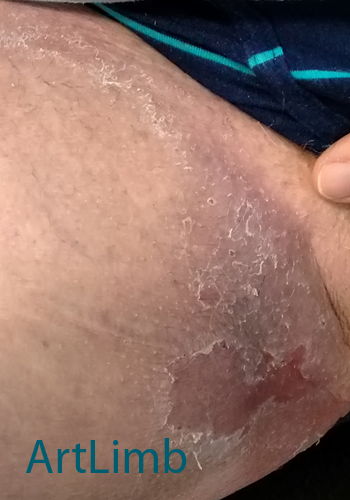
Fungal infection can be quite common and are usually superficial and mild, without obvious irritating symptoms. These must be treated by medical specialist only.
The photo above shows an example of a fungal infection.
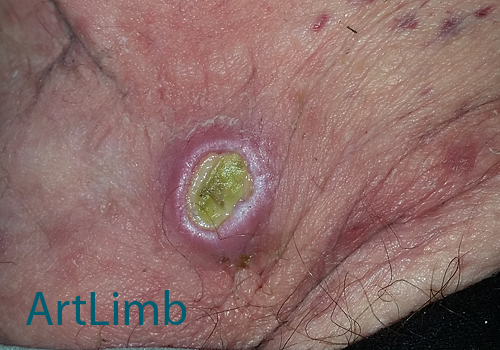
Ulcer is an open sore which erodes away the skin of the stump. There are several medical conditions (local blood circulation disorder, diabetes, etc) and prosthetic issues (areas of high pressure in the socket, etc) that can lead to ulcers forming. Ulcers need to be treated by a medical professional and be seen by a prosthetist to determine if a socket adjustment is required.
In general ulcers are slow to heal and need to be unloaded.
The photo above shows an example of an ulcer on the stump.
During the preparation of this article we used information from the QALS (Queensland Artificial Limb Service) information handbook “Information for people living with amputation” with permission from the QALS manager.

Great work – so informative and of real benefit. Thanks for your ongoing support !
Thanks Cathy! Glad to know you are getting benefit from the articles.
Cheers,
ArtLimb team
Fantastic article. As someone who is facing a below knee amputation, this article is fantastic in highlighting what issues I may need to be aware of. I’d love to see an article on what people experience as they get older. I.e how does age effect wearing a prothetic.
Thanks for the great information.
Hi Sarah. Thank you very much for your feedback. We understand your concern about how your body will adapt to wearing a prosthetic limb and how this will change over time.
This question is brilliant, and we have started working on a selection of articles to cover this.
In the mean time, the information in the LOWER LIMB (overview) section covers the initial stages of getting fitted with a limb and is a good place to start.
Thanks again for your support,
ArtLimb team